The Musculoskeletal Conundrum
Musculoskeletal (MSK) (muscles, joints, bones) conditions will inevitably affect a majority of individuals at some point in their lives. Whether it be generalized back pain, arthritis, disc herniation, an ankle sprain, or something else altogether, chances are you'll find yourself in a doctor's office seeking help to get over you pain and symptoms.
The problem is, with so many different healthcare providers that treat MSK complaints, who would be the best provider for your condition?
Answer: Any qualified MSK provider that focuses on evidence based, patient centered care.
I know, I know. It's not the most specific answer. I'm sure you were thinking I'd say a chiropractor, because I am one. Well, guess what? There are plenty of chiros I wouldn't recommend seeing. In my opinion, any DC, DPT, MD, DO, etc. that keeps up with current best practice guidelines regarding MSK healthcare is likely a good choice for you. Likewise, any of the above mentioned providers that still treat all MSK patients the same way as they have for the past 10+ years would probably be a bad choice for your healthcare.
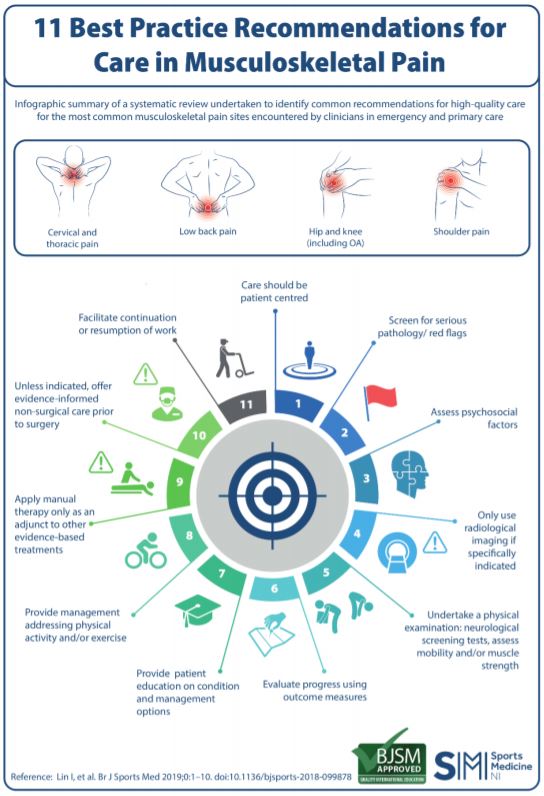
What does good MSK healthcare look like you ask? In 2019, the British Journal of Sports Medicine published "11 Best Practice Recommendations for Care in Musculoskeletal Pain." This paper outlines 11 key points for current, quality, evidence based MSK healthcare.
Check it out:
- Patient centered care - Every patient is different. Different situations, expectations, histories, experiences, preferences, etc. Care should be individually tailored to each individual patient.
- Screen for serious pathology/red flags - We need to make sure that your symptoms aren't a result of something that needs immediate emergency medical intervention. It's rare, but should be considered in order to be safe.
- Assess psychosocial factors - Current research is showing more and more that pain is more complex than just injured tissue. Our emotions, expectations, and perceptions also play a role in how we experience pain.
- Only use radiological imaging if specifically indicated - "Taking a picture" (x-ray, MRI, CT) just because something hurts is bad practice, a waste of resources, and may lead to unnecessary and/or ineffective interventions. There are clear guidelines of when imaging is appropriate, yet all too often it's one of the first things being done.
- Physical examination assessing neuro tests and mobility and/or strength - Ever been examined for your back pain by a doctor on the other side of the room and he/she never actually touched you or had you move off the table? This doesn't cut it.
- Evaluate progress using outcome measures - How do you know treatment is working well enough if you don't keep track of outcomes? Pain itself is a poor indicator of functional health and should not be the basis to determine "success."
- Patient education - Do you want to have to rely on your doctor every time your back flares up? Or, do you want to learn ways you can help take care of yourself?
- Physical activity and/or exercise - Movement complaints require movement solutions. There's no pill, patch, or passive therapy that can result in true improvement and correction. You have to learn to move if you're going to get over MSK pain.
- Manual therapy used WITH other evidence based treatments - I'm a chiro. I love joint manipulation. Chiros aren't the only providers who utilize this treatment method. PTs and DOs regularly use it too. However, joint manipulation by itself does not provide long term results. If it's not paired with rehab and selfcare education, you'll start to understand why people think you have to see a chiropractor forever.
- Unless indicated, surgery should be a last resort - Why on earth would you submit to the scalpel when there may be several other non-surgical treatment options? Think high risk vs low risk. Surgery is appropriate when it's appropriate.
- Facilitate continuation or resumption of work - Some of the worst MSK advice you could be given is "just rest and stop doing everything until the pain goes away." The better you can adapt and improve to normal day to day demands, the sooner you'll be feeling and moving well.
Does your doctor follow along with the recommendations outlined above?
If not, it may be time to find a new doctor.
I'm Dr. Andrew Kubosumi, DC. I'm an evidence based chiropractor in Mesquite, TX. I'll help you overcome your MSK related complaints and teach you how to take care of yourself.
References:
- Lin I, Wiles L, Waller R, et alWhat does best practice care for musculoskeletal pain look like? Eleven consistent recommendations from high-quality clinical practice guidelines: systematic review British Journal of Sports Medicine 2020;54:79-86.
Dr. Andrew Kubosumi
Contact Me